Gastric Sleeve explained in detail
- Why undergo gastric sleeve surgery?
- How is gastric sleeve surgery performed?
- Cost factors of gastric sleeve surgery
- Differences between gastric sleeve and gastric bypass
- What are the benefits of gastric sleeve surgery?
- Who is a suitable candidate for gastric sleeve surgery?
- What lifestyle changes are needed after gastric sleeve surgery?
- Traveling abroad for gastric sleeve surgery
- How long do results from gastric sleeve surgery last?
- Common myths about gastric sleeve surgery
- Preoperative preparation for gastric sleeve surgery
- Nutritional guidelines after gastric sleeve surgery
- Key vitamins and supplements after gastric sleeve
- Exercise recommendations after gastric sleeve
- Hydration strategies after gastric sleeve
- Hospital stay and immediate recovery
- Long-term dietary strategies after gastric sleeve
- Potential risks and complications of gastric sleeve
- Impact of gastric sleeve on fertility and pregnancy
- How to choose a gastric sleeve clinic
- Gastric sleeve and remission of type 2 diabetes
- Post-surgery follow-up care
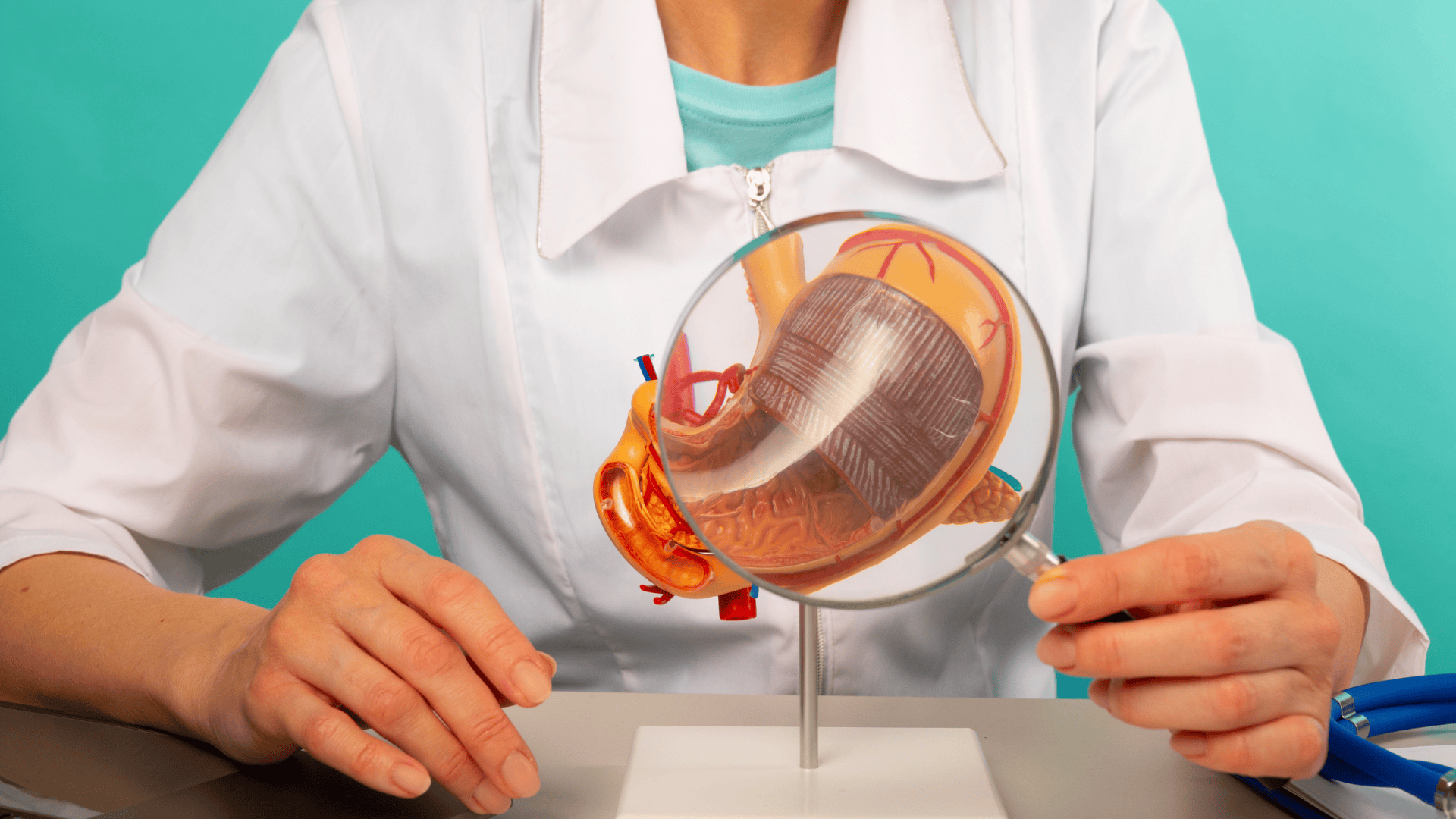
A gastric sleeve, also known as sleeve gastrectomy, is a surgical procedure designed for weight loss. During this operation, a significant portion of the stomach is removed, transforming the stomach into a narrow tube or "sleeve." This results in a drastically reduced stomach capacity, which means that patients can consume less food.
The procedure is often recommended for individuals suffering from obesity who have not achieved success with other weight loss methods, such as diet and exercise. By reducing the size of the stomach, patients experience a quicker sensation of fullness, leading to decreased caloric intake. Additionally, the surgery affects the production of certain hormones that regulate appetite, which can further help to reduce hunger.
A gastric sleeve, also known as sleeve gastrectomy, is a surgical procedure designed for weight loss.
Gastric sleeve surgery can be performed laparoscopically, meaning it is conducted through small incisions using a camera and specialized instruments. This minimally invasive approach reduces recovery time and lowers the risk of complications. However, like any surgical procedure, there are risks associated with a gastric sleeve, including infections, bleeding, and digestive complications.
After the surgery, patients must make significant dietary and lifestyle adjustments. This typically involves following a specific diet that starts with liquid foods and gradually progresses to solid foods. Regular follow-ups with healthcare providers are essential to monitor progress and identify any potential complications early.
Overall, a gastric sleeve can be an effective solution for long-term weight loss and may improve the quality of life for patients, provided it is combined with a healthy lifestyle and changes in eating behavior.

Why undergo gastric sleeve surgery?
Gastric sleeve surgery, also known as sleeve gastrectomy, is often chosen by individuals seeking a significant and lasting solution to obesity when traditional methods such as diet and exercise have not been successful. This procedure is usually recommended for people with a body mass index (BMI) of 40 or higher, or for those with a BMI of 35 or higher who are experiencing serious health problems related to obesity, such as type 2 diabetes, hypertension, or sleep apnea.
The surgery works by permanently reducing the size of the stomach, which helps people feel fuller faster and reduces the amount of food they can eat. Many opt for the gastric sleeve as it offers a more straightforward procedure than gastric bypass and avoids some of the potential complications related to nutrient absorption, as it doesn’t involve rerouting the intestines.
Gastric sleeve surgery, also known as sleeve gastrectomy, is often chosen by individuals seeking a significant and lasting solution to obesity when traditional methods such as diet and exercise have not been successful.
It is particularly appealing because it leads to significant weight loss, which not only improves physical health but can also greatly enhance quality of life, boosting self-esteem, mobility, and energy levels. For many, it represents a second chance at regaining control over their weight and health, reducing the risks of life-threatening conditions, and promoting long-term wellness.
How is gastric sleeve surgery performed?
Gastric sleeve surgery is performed using a minimally invasive technique called laparoscopy, which involves making small incisions in the abdomen through which a camera and surgical tools are inserted. The surgeon removes approximately 75-80% of the stomach, leaving behind a small, tube-shaped portion that resembles a banana. This new, smaller stomach drastically limits the amount of food a person can eat, but it still functions normally, allowing food to pass through the digestive tract as it would naturally.
**Gastric sleeve surgery is performed using a minimally invasive technique called laparoscopy, which involves making small incisions in the abdomen through which a camera and surgical tools are inserted.
One of the key aspects of the procedure is that it also reduces the production of the hunger hormone ghrelin, which helps to decrease appetite, making it easier for individuals to stick to smaller portions. Unlike gastric bypass surgery, the intestines are not altered, so there is no malabsorption of nutrients, making it a simpler operation with fewer risks of nutritional deficiencies.
The entire procedure usually takes about one to two hours, and most patients stay in the hospital for a couple of days for monitoring. After surgery, patients follow a strict diet, gradually transitioning from liquids to solid foods, and must adopt lifelong changes to their eating habits and lifestyle in order to maintain their weight loss and overall health.
Cost factors of gastric sleeve surgery
The price of gastric sleeve surgery can vary widely depending on location, surgeon experience, and hospital facilities. In general, costs include:
💚 Surgeon and anesthesia fees
💚 Hospital stay and operating room expenses
💚 Preoperative tests and consultations
💚 Postoperative medications and supplements
💚 Follow-up appointments and long-term care
Understanding these factors helps patients plan financially and avoid unexpected costs.
Differences between gastric sleeve and gastric bypass
Although both procedures are popular bariatric surgeries, gastric sleeve and gastric bypass differ significantly. Gastric sleeve involves removing part of the stomach, while gastric bypass creates a small stomach pouch and reroutes the intestines. This means gastric bypass carries a higher risk of nutrient malabsorption but can sometimes lead to greater weight loss. In contrast, gastric sleeve offers a simpler structure with fewer long-term complications, making it an attractive choice for many patients.
What are the benefits of gastric sleeve surgery?
The benefits of gastric sleeve surgery are both profound and wide-ranging, making it one of the most popular bariatric procedures today. One of the primary benefits is the significant weight loss that patients typically experience in the months and years following surgery. Many individuals lose 50-60% of their excess weight within the first year, which leads to improvements in a variety of obesity-related health conditions. For example, many patients see dramatic reductions in type 2 diabetes, with some experiencing complete remission.
The benefits of gastric sleeve surgery are both profound and wide-ranging, making it one of the most popular bariatric procedures today.
Conditions like high blood pressure, high cholesterol, and sleep apnea also tend to improve or resolve entirely after weight loss, reducing the need for medications and lowering the risks of heart disease and stroke. Additionally, because the stomach is reduced in size and the hormone ghrelin is decreased, patients feel less hungry, which helps them maintain long-term weight loss without feeling deprived.
Beyond the physical health benefits, there are significant psychological and social improvements. Many patients report increased self-confidence, reduced anxiety, and a greater willingness to engage in social and physical activities that were once too challenging due to their weight.
The improvement in mobility also allows for more physical activity, which further supports healthy weight maintenance and contributes to a more active and fulfilling lifestyle. Although the surgery requires a strong commitment to dietary changes and regular exercise, the benefits of gastric sleeve surgery often extend far beyond the weight loss itself, enhancing overall quality of life and promoting a healthier, longer future.
Who is a suitable candidate for gastric sleeve surgery?
Gastric sleeve surgery is typically recommended for individuals who are significantly overweight or obese and have struggled to lose weight through traditional methods such as diet, exercise, or medication. Ideal candidates usually have a Body Mass Index (BMI) of 40 or higher, or a BMI of 35 or more with obesity-related health conditions like type 2 diabetes, hypertension, joint pain, or sleep apnea. It is also important that candidates are mentally prepared for the lifestyle changes required after surgery. Those considering the procedure should be willing to commit to a long-term health plan involving nutritious eating, physical activity, and regular medical follow-ups.
Gastric sleeve surgery is typically recommended for individuals who are significantly overweight or obese and have struggled to lose weight through traditional methods such as diet, exercise, or medication.
In addition, candidates must be free of any medical or psychological conditions that would make the surgery unsafe or ineffective. A thorough evaluation by a bariatric team—including a surgeon, dietitian, and sometimes a psychologist—is essential to determine if gastric sleeve surgery is the right fit.

What lifestyle changes are needed after gastric sleeve surgery?
Success after gastric sleeve surgery relies heavily on making permanent lifestyle changes. In the first few weeks following the procedure, patients follow a staged diet that begins with clear liquids, progresses to pureed foods, and then eventually reintroduces solid foods. Over time, patients are expected to adopt a high-protein, low-carb diet, eat small meals, chew food thoroughly, and avoid sugary or carbonated beverages. Regular physical activity is also critical—not only for continued weight loss, but also for building strength, improving heart health, and supporting mental well-being.
Patients should aim for at least 150 minutes of moderate exercise per week once fully recovered. Additionally, lifelong vitamin and mineral supplementation is often required to prevent deficiencies. Routine check-ups with healthcare providers are essential to monitor nutritional status, weight trends, and overall health. While the surgery provides a powerful tool for weight loss, long-term success depends on a deep commitment to healthier habits.
Traveling abroad for gastric sleeve surgery
An increasing number of people choose to undergo gastric sleeve surgery abroad due to lower costs and access to experienced surgeons. Popular destinations include Turkey, Mexico, and Eastern Europe, where specialized clinics offer comprehensive packages. Patients considering this option should carefully review the clinic’s credentials, language support, and follow-up care plans to ensure safety and continuity of treatment.
How long do results from gastric sleeve surgery last?
The results of gastric sleeve surgery can be long-lasting and life-changing, particularly when accompanied by a consistent, healthy lifestyle. Most patients experience their greatest weight loss in the first 12 to 18 months, often losing 50–70% of their excess weight. After this initial period, weight typically stabilizes, although some individuals may regain a small amount if they slip back into unhealthy eating habits.
However, long-term studies have shown that many patients are able to maintain substantial weight loss even five to ten years post-surgery. What’s more, improvements in health conditions such as type 2 diabetes and high blood pressure often persist over the long term. Maintaining regular follow-up care, attending support groups, and continuing to prioritize nutritious food and exercise are all vital components of lasting success.
Common myths about gastric sleeve surgery
There are several myths and misconceptions about gastric sleeve surgery that can lead to confusion. One common myth is that it’s an “easy way out” or a cosmetic fix—when in reality, gastric sleeve surgery is a medically recognized treatment for obesity, and it requires lifelong commitment and discipline. Another misconception is that patients will never be able to eat normally again. While portion sizes are permanently reduced, individuals can enjoy a wide variety of foods once fully recovered—just in smaller, more mindful quantities.
There are several myths and misconceptions about gastric sleeve surgery that can lead to confusion.
Some also believe that weight loss is guaranteed, but the truth is that success depends on active patient participation. Finally, there is a belief that the procedure is dangerous; however, while all surgeries carry some risk, gastric sleeve surgery is considered safe and effective, especially when performed by an experienced bariatric surgeon. Education and support are key to setting realistic expectations and achieving positive, lasting results.
Preoperative preparation for gastric sleeve surgery
Before undergoing gastric sleeve surgery, patients must complete several important steps to ensure safety and maximize results. Surgeons often request a series of medical evaluations, including blood tests, imaging, and sometimes heart or lung assessments. A supervised pre-surgery diet may be required to reduce liver size, making the operation safer. Patients are usually advised to quit smoking, limit alcohol, and stop certain medications that could interfere with healing. Education about the procedure, risks, and postoperative expectations is also crucial, as well-informed patients are more likely to succeed in the long run.
Nutritional guidelines after gastric sleeve surgery
Maintaining proper nutrition is one of the cornerstones of success following gastric sleeve surgery. Because the stomach is smaller, it cannot hold large amounts of food, so every bite must count. Protein intake becomes the top priority, followed by vegetables, fruits, and whole grains. Patients are encouraged to avoid high-sugar and high-fat foods that can slow down weight loss or trigger digestive discomfort. Hydration is equally important, but liquids should be consumed between meals rather than during them to prevent the small stomach from overfilling.

Key vitamins and supplements after gastric sleeve
After a gastric sleeve, patients may not absorb all the nutrients they need from food alone, which makes supplementation vital. Commonly prescribed supplements include:
💚 A complete multivitamin with minerals
💚 Vitamin B12, often in sublingual or injection form
💚 Vitamin D and calcium to support bone health
💚 Iron, especially for women of childbearing age
💚 Folic acid, depending on individual needs
Following the supplement plan recommended by the healthcare team helps prevent deficiencies and supports long-term health.
Exercise recommendations after gastric sleeve
Physical activity is an essential part of recovery and long-term success after gastric sleeve surgery. Initially, patients may start with light walking just days after the procedure to promote circulation and reduce the risk of blood clots. Over time, activity should progress to more structured exercises such as strength training, swimming, or cycling. Building muscle not only improves metabolism but also helps maintain weight loss. A gradual, consistent exercise routine provides the best results without overwhelming the body during recovery.
Hydration strategies after gastric sleeve
Staying hydrated is a common challenge for patients after gastric sleeve surgery because the stomach’s reduced size limits liquid intake. To avoid dehydration, patients should:
💚 Sip water slowly throughout the day instead of drinking large amounts at once
💚 Aim for 1.5 to 2 liters of fluid daily, as recommended by their doctor
💚 Avoid carbonated beverages that cause bloating
💚 Limit caffeine and alcohol, which can dehydrate the body
💚 Incorporate clear broths or herbal teas to add variety
Consistent hydration supports recovery, digestion, and overall well-being.
Hospital stay and immediate recovery
Most patients remain in the hospital for one to three days following gastric sleeve surgery. During this time, the medical team monitors vital signs, manages pain, and ensures the digestive system is adapting to the new stomach structure. Patients typically begin sipping clear liquids within 24 hours and are encouraged to walk short distances in the hospital corridors. Early mobilization reduces complications and speeds up recovery.
Long-term dietary strategies after gastric sleeve
Years after gastric sleeve surgery, dietary habits remain central to maintaining results. Patients are advised to focus on lean proteins, high-fiber vegetables, and nutrient-rich foods. Portion control becomes second nature, but occasional indulgences are acceptable as long as balance is maintained. Avoiding grazing or snacking on calorie-dense foods helps prevent weight regain. Patients who prioritize nutrition often enjoy stable results for a lifetime.
Potential risks and complications of gastric sleeve
While considered safe, gastric sleeve surgery does involve certain risks. These may include:
💚 Leakage along the staple line of the stomach
💚 Infection at the incision sites
💚 Blood clots in the legs or lungs
💚 Strictures or narrowing of the stomach sleeve
💚 Nutritional deficiencies if supplements are neglected
Choosing an experienced bariatric surgeon and adhering to medical advice greatly reduces these risks.
Impact of gastric sleeve on fertility and pregnancy
Women who undergo gastric sleeve surgery often notice improvements in fertility, as weight loss can regulate hormonal imbalances and menstrual cycles. However, doctors generally recommend waiting 12 to 18 months before attempting pregnancy. This period allows weight and nutrition to stabilize, ensuring a safer environment for both mother and baby. With proper planning and medical supervision, pregnancy after gastric sleeve can be healthy and successful.
How to choose a gastric sleeve clinic
Selecting the right clinic for gastric sleeve surgery is a crucial decision. Patients should look for:
💚 Surgeons with specialized bariatric experience and certifications
💚 Modern facilities equipped with advanced laparoscopic technology
💚 Comprehensive pre- and post-surgery support programs
💚 Transparent pricing and clear explanations of costs
💚 Positive outcomes and published success rates
Researching and comparing clinics helps patients feel confident in their choice and ensures the highest standard of care.
Gastric sleeve and remission of type 2 diabetes
One of the most powerful medical benefits of gastric sleeve surgery is its effect on type 2 diabetes. Many patients see their blood sugar levels improve significantly, with some achieving complete remission. Weight loss reduces insulin resistance, while hormonal changes after surgery further support blood sugar control. These improvements often occur within weeks of surgery, even before major weight loss has taken place.
Post-surgery follow-up care
Regular follow-up visits are an essential part of the recovery process after gastric sleeve surgery. These appointments allow doctors to monitor weight loss, check for complications, and adjust supplements or medications as needed. Follow-ups are usually scheduled at one week, one month, three months, six months, and annually thereafter. Consistent check-ins ensure patients remain on track with their health goals.


