Gastric reduction explained in detail
- Why undergo gastric reduction surgery?
- Different surgical techniques in gastric reduction
- How to prepare for gastric reduction surgery
- How is gastric reduction surgery performed?
- What are the benefits of gastric reduction surgery?
- Potential risks and side effects
- Differences between gastric sleeve and gastric bypass
- Who qualifies for gastric reduction surgery?
- What to expect long-term after gastric reduction surgery
- Traveling for gastric reduction surgery
- Life after gastric reduction surgery: Daily routines and changes
- Common misconceptions about gastric reduction surgery
- Nutritional adjustments after surgery
- Importance of hydration
- Exercise after gastric reduction
- Supplements required after gastric reduction
- Role of follow-up appointments
- Impact on fertility and pregnancy
- Lifestyle changes before surgery
- Gastric reduction and diabetes management
- Emotional adjustments to lifestyle changes
- Long-term weight maintenance strategies
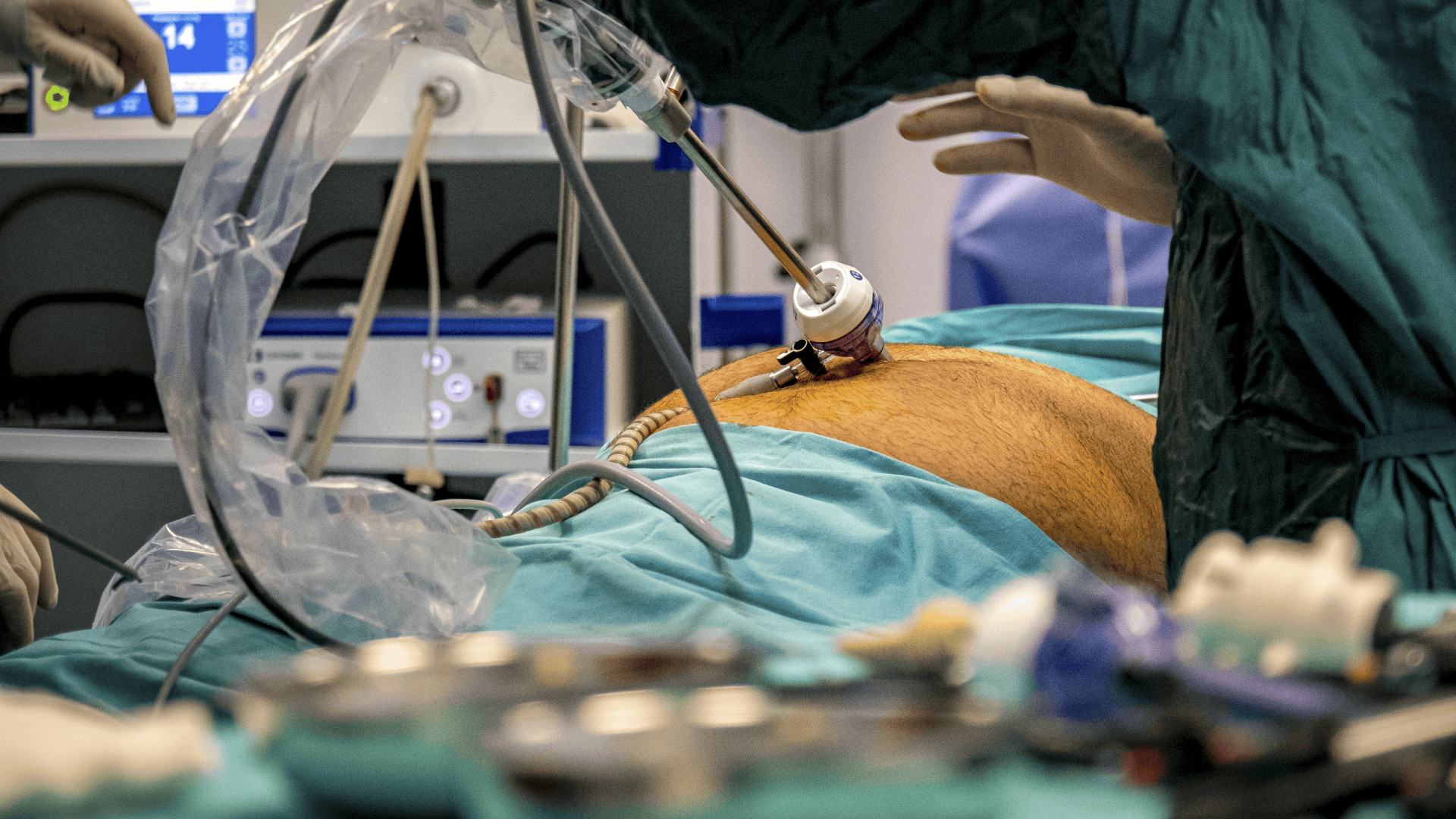
A gastric reduction, also known as bariatric surgery, is a surgical procedure performed to reduce the size of the stomach, with the aim of promoting weight loss in people with severe obesity. By reducing the stomach’s capacity, a person is able to eat less food and feels full more quickly, which ultimately results in consuming fewer calories and losing weight.
There are several methods of performing a gastric reduction. In a gastric bypass, the stomach is not only reduced in size but part of the small intestine is also bypassed, leading to reduced food intake as well as decreased nutrient absorption. In a gastric sleeve procedure, a large portion of the stomach is removed, leaving behind a narrow, tube-like stomach. Another option is the gastric band, where an adjustable band is placed around the upper part of the stomach, dividing it into two sections, making the person feel full after consuming smaller amounts of food.
A gastric reduction, also known as bariatric surgery, is a surgical procedure performed to reduce the size of the stomach, with the aim of promoting weight loss in people with severe obesity.
Gastric reduction is primarily intended for people with severe obesity who have not been successful with other methods like dieting or exercise. It is often recommended for individuals with a BMI of 40 or higher, or for those with a BMI of 35 who also suffer from other health conditions such as diabetes or high blood pressure. While the surgery often results in significant weight loss and improvements in obesity-related conditions, it also carries risks. Complications like infections, bleeding, and nutrient deficiencies can occur. After the procedure, it is essential to make lifelong changes in lifestyle and diet to maintain the weight loss and avoid health issues.

Why undergo gastric reduction surgery?
Gastric reduction surgery, or bariatric surgery, is often considered when traditional weight loss methods like dieting and exercise have not been successful. People with severe obesity, especially those with a BMI of 40 or higher, or with a BMI of 35 and associated health issues like diabetes or hypertension, may opt for this surgery to improve their health and quality of life.
The primary goal is to facilitate weight loss by physically altering the digestive system, which helps reduce food intake and, in some cases, changes how the body absorbs nutrients. For individuals struggling with the psychological and physical burdens of obesity, this surgery can offer a renewed sense of control over their bodies and health. Obesity is often linked to various chronic diseases, including heart disease, type 2 diabetes, sleep apnea, and joint problems.
For many, gastric reduction is not just about appearance; it’s about drastically improving or even saving their lives. It helps them combat these life-threatening conditions, increases life expectancy, and enhances overall mobility and energy levels. Moreover, the decision to undergo surgery is also deeply personal, often fueled by a desire to regain confidence, reduce stigma, and improve mental well-being.
Different surgical techniques in gastric reduction
While gastric bypass and sleeve gastrectomy are the most common, there are other surgical approaches available depending on the patient’s condition and goals. For example, biliopancreatic diversion with duodenal switch is a more complex surgery that combines restriction with significant malabsorption, leading to powerful weight loss results but also requiring strict lifelong nutritional follow-up. Surgeons determine the best option by evaluating a patient’s health history, BMI, and co-existing conditions, ensuring the most effective and safest procedure is chosen.
How to prepare for gastric reduction surgery
Preparation for gastric reduction surgery often begins weeks before the procedure. Patients are usually placed on a pre-surgery diet to shrink the liver and reduce surgical risks. Medical evaluations such as blood tests, imaging, and consultations with dietitians and psychologists are also part of the process. In addition, patients are encouraged to quit smoking, reduce alcohol intake, and start practicing smaller meal portions to ease the transition. Proper preparation ensures better outcomes and smoother recovery.
How is gastric reduction surgery performed?
Gastric reduction surgery involves reducing the stomach's size to limit food intake, and this can be done through different procedures, the most common being gastric bypass, sleeve gastrectomy, and adjustable gastric banding. Each method has its unique approach but shares the core principle of restricting how much food the stomach can hold.
In a gastric bypass, surgeons create a small pouch from the stomach and directly connect it to the small intestine, effectively bypassing a large part of the stomach and small bowel, which reduces both food intake and nutrient absorption. Sleeve gastrectomy involves removing a large portion of the stomach, leaving behind a tube-shaped stomach or "sleeve" that significantly reduces its capacity. Adjustable gastric banding, on the other hand, places an inflatable band around the upper part of the stomach, creating a small pouch above the band that limits food intake.
Gastric reduction surgery involves reducing the stomach's size to limit food intake, and this can be done through different procedures, the most common being gastric bypass, sleeve gastrectomy, and adjustable gastric banding.
These procedures are typically performed using minimally invasive techniques, such as laparoscopic surgery, which involves small incisions and the use of a camera and surgical tools. Recovery is generally quicker, with less pain and scarring compared to open surgery. Patients are required to follow specific dietary guidelines post-surgery, gradually moving from liquids to solid foods, and must commit to long-term lifestyle changes to achieve lasting results.
What are the benefits of gastric reduction surgery?
The benefits of gastric reduction surgery extend beyond significant and sustained weight loss. For many patients, this type of surgery offers a pathway to better overall health by addressing and sometimes reversing obesity-related conditions. Weight loss achieved through surgery can lead to the improvement or resolution of type 2 diabetes, which is often one of the most significant outcomes for those with this condition.
The benefits of gastric reduction surgery extend beyond significant and sustained weight loss.
Patients frequently experience lower blood pressure and cholesterol levels, reducing the risk of heart disease and stroke. Sleep apnea, a common issue in individuals with obesity, is also significantly alleviated or completely resolved after surgery, leading to better sleep and increased energy during the day. Additionally, the reduction in joint pain and improvement in mobility allows patients to engage in physical activities that were previously too difficult due to their weight, further contributing to overall well-being.
Beyond physical health, many individuals experience a profound improvement in their mental health after surgery. Losing weight can enhance self-esteem, reduce anxiety and depression, and foster a greater sense of control over one’s life. Furthermore, the surgery helps mitigate the social stigmas associated with obesity, providing individuals with more confidence in social and professional settings. While it requires ongoing commitment, gastric reduction surgery can be life-changing, both in terms of health outcomes and quality of life.
Potential risks and side effects
Although considered safe, gastric reduction surgery is still a major procedure with possible risks. Short-term complications may include infection, bleeding, or adverse reactions to anesthesia. Long-term issues can include dumping syndrome, gallstones, or strictures.
💚 Following all dietary guidelines
💚 Attending regular medical check-ups
💚 Reporting any unusual symptoms early
By working closely with healthcare professionals, most risks can be managed or avoided.
Differences between gastric sleeve and gastric bypass
Though both procedures aim to reduce food intake, there are key distinctions. Gastric sleeve removes a large portion of the stomach, permanently reducing its size. Gastric bypass, however, not only reduces the stomach but also reroutes part of the intestine, leading to less calorie absorption. Patients who need more significant weight loss or have severe metabolic conditions may benefit from bypass, while those seeking a simpler, purely restrictive method may choose the sleeve.
Who qualifies for gastric reduction surgery?
Gastric reduction surgery is typically recommended for individuals who are severely obese and have not achieved success through non-surgical weight loss methods, such as diet, exercise, or medication. The most common criteria include a Body Mass Index (BMI) of 40 or higher, or a BMI of 35 or more in combination with serious obesity-related conditions, such as type 2 diabetes, high blood pressure, heart disease, or sleep apnea. However, eligibility isn’t just based on numbers—patients also undergo a thorough evaluation of their physical health, psychological readiness, and commitment to long-term lifestyle changes.
Candidates must be willing to engage in lifelong follow-up care, including nutritional counseling, exercise routines, and regular check-ins with medical professionals. Each case is unique, and suitability is always determined in collaboration with a multidisciplinary medical team.
What to expect long-term after gastric reduction surgery
Long-term success after gastric reduction surgery depends largely on a patient’s ability to maintain consistent lifestyle changes and follow-up care. In the years following the procedure, many patients maintain a 50–70% loss of excess weight, significantly improving their overall health. While the majority of weight loss happens within the first 12–18 months, sustained results are common when healthy habits are continued.
Regular physical activity, mindful eating, and proper nutrition are essential to prevent weight regain. Many patients also require lifelong vitamin and mineral supplementation, especially after gastric bypass, due to altered digestion and nutrient absorption. Mental health support may also be beneficial, as adjusting to a new body image and lifestyle can be emotionally complex. With commitment and support, gastric reduction surgery can provide lasting physical and emotional transformation.
Traveling for gastric reduction surgery
Medical tourism has become increasingly popular, with patients traveling abroad for gastric reduction procedures due to affordability and access to highly skilled surgeons. Countries with advanced bariatric centers often offer comprehensive packages that include surgery, accommodation, and aftercare.
💚 Lower overall treatment costs
💚 Access to internationally trained specialists
💚 Shorter waiting times compared to home countries
For those considering this option, careful research and choosing accredited clinics is essential.
Life after gastric reduction surgery: Daily routines and changes
Daily life after gastric reduction surgery involves a new approach to eating, activity, and self-care. Patients must adapt to smaller meal portions, eat slowly, and chew thoroughly to avoid discomfort and promote digestion. Hydration becomes especially important, but drinking should be timed separately from meals to prevent stretching the stomach or feeling overly full.
A protein-rich diet with limited sugars and processed foods is key to maintaining energy and muscle mass while continuing to lose weight. Physical activity becomes a regular part of the routine—starting with gentle walking post-surgery and eventually progressing to more structured exercise. Emotionally, many people report feeling more confident, energetic, and socially engaged, but support groups and counseling can help with challenges like food cravings, body image adjustments, or emotional eating. Over time, these changes become part of a healthier, more fulfilling lifestyle.
Common misconceptions about gastric reduction surgery
There are many misconceptions surrounding gastric reduction surgery, which can create unnecessary fear or unrealistic expectations. A common myth is that the surgery is a “quick fix” or an “easy way out,” when in fact, it’s a serious medical procedure that requires lifelong commitment and lifestyle change.
There are many misconceptions surrounding gastric reduction surgery, which can create unnecessary fear or unrealistic expectations.
Another misunderstanding is that patients won’t be able to eat normally again—while food volume is reduced, patients can still enjoy a wide variety of foods in moderation. Some also believe weight loss is guaranteed, but long-term results depend heavily on behavioral changes and follow-up care.
There’s also concern about safety; while all surgeries carry risk, bariatric procedures are considered safe and effective, especially with modern minimally invasive techniques. Debunking these myths is essential for helping people make informed, confident decisions about their health.
Nutritional adjustments after surgery
After gastric reduction, patients need to adapt to a new way of eating that focuses on nutrient-dense foods. Portion sizes are smaller, and meals must be planned carefully to ensure that protein, vitamins, and minerals are consumed consistently. Because the stomach can no longer accommodate large meals, every bite matters. Patients are encouraged to prioritize lean protein, vegetables, and whole foods, while avoiding empty calories that can hinder progress. Over time, these dietary adjustments become second nature and contribute to lasting success.
Importance of hydration
Hydration plays a crucial role after gastric reduction surgery. Patients are advised to sip water throughout the day rather than drinking large quantities at once, as the smaller stomach cannot hold much fluid. Beverages should be sugar-free and non-carbonated, and drinking during meals should be avoided to prevent discomfort or stretching of the stomach. Staying well-hydrated helps with digestion, supports metabolism, and prevents fatigue, making it a cornerstone of long-term recovery and weight maintenance.
Exercise after gastric reduction
Physical activity is gradually introduced after surgery to support weight loss and overall health. Initially, walking is encouraged within the first few days, which helps circulation and speeds up recovery. As healing progresses, patients can add low-impact exercises like swimming, cycling, or yoga. Eventually, strength training becomes important for building muscle and preventing the loss of lean body mass. Exercise not only burns calories but also boosts mood, energy, and cardiovascular health.

Supplements required after gastric reduction
Following surgery, the body’s ability to absorb nutrients changes, making supplementation essential. Patients are typically advised to take multivitamins, vitamin B12, iron, calcium, and vitamin D. These supplements prevent deficiencies that could otherwise lead to fatigue, bone weakness, or anemia.
💚 Daily intake of prescribed vitamins
💚 Regular blood tests to monitor nutrient levels
💚 Adjustments based on individual health needs
Maintaining these habits is key to long-term wellness and preventing complications.
Role of follow-up appointments
Regular follow-up visits with the medical team are critical for monitoring progress and preventing complications. Surgeons and dietitians track weight loss, nutritional status, and overall health while also addressing any concerns the patient may have. These appointments allow early detection of problems like nutrient deficiencies or weight regain. Consistent follow-up care ensures patients stay on track and achieve the full benefits of their surgery.
Impact on fertility and pregnancy
For women of childbearing age, gastric reduction can have a positive effect on fertility by restoring regular ovulation and reducing obesity-related complications. Doctors usually recommend waiting 12 to 18 months after surgery before becoming pregnant, ensuring the body stabilizes at a healthier weight and nutrient levels are balanced. With proper monitoring and supplementation, many women experience safer pregnancies and healthier outcomes for both mother and baby.

Lifestyle changes before surgery
Making adjustments before the procedure can significantly impact success afterward. Patients are encouraged to establish healthier eating habits, reduce sugary foods, and begin exercising, even in small amounts.
💚 Eating smaller, balanced meals
💚 Reducing processed and fried foods
💚 Practicing mindful eating
💚 Increasing daily physical activity
These steps not only prepare the body for surgery but also make post-operative transitions much smoother.
Gastric reduction and diabetes management
One of the most profound benefits of gastric reduction is its effect on type 2 diabetes. Many patients experience rapid improvements in blood sugar levels, often within days of surgery, even before significant weight loss occurs. For some, this leads to reduced dependence on medication or even complete remission of diabetes. Long-term success, however, depends on maintaining a healthy lifestyle and attending regular follow-ups with endocrinologists.
Emotional adjustments to lifestyle changes
Although the psychological aspects aren’t the main focus here, it’s important to acknowledge that adapting to a new lifestyle can feel challenging at times. Patients need patience as they develop new routines with eating, exercising, and daily care. Support from family and structured medical guidance helps ease this transition, ensuring long-term adherence and better outcomes.
Long-term weight maintenance strategies
Weight loss after gastric reduction is most rapid during the first year, but keeping it off requires ongoing strategies.
💚 Maintaining regular exercise routines
💚 Prioritizing protein-rich foods
💚 Avoiding grazing or snacking on high-calorie foods
💚 Continuing follow-up with dietitians
Sustaining these habits helps ensure that weight loss is not only achieved but also preserved for life.


