
Capsular Contracture Correction explained in detail
- Why undergo Capsular Contracture Correction?
- How is Capsular Contracture Correction performed?
- Advanced Techniques in Capsular Contracture Correction
- Risks Associated with Capsular Contracture Correction
- Ideal Candidates for Capsular Contracture Correction
- Choosing the Right Implant During Correction Surgery
- What are the benefits of Capsular Contracture Correction?
- Understanding Costs of Capsular Contracture Correction
- Signs and Symptoms of Capsular Contracture
- Preventing Capsular Contracture After Breast Surgery
- Choosing the Right Surgeon for Capsular Contracture Correction
- What to Expect During Recovery from Correction Surgery
- Post-Surgical Care Tips for Capsular Contracture Correction
- Non-Surgical Options to Delay Capsular Contracture
- Recovery Timeline After Capsular Contracture Correction
- Impact of Implant Placement on Capsular Contracture
- Innovations in Capsular Contracture Treatment
- Capsular Contracture Correction for Reconstruction Patients
- Preventing Recurrence of Capsular Contracture
- Long-Term Considerations After Correction Surgery
- Capsular Contracture Correction in Complex Cases
- Role of Antibiotics in Capsular Contracture Correction
Capsular contracture correction is a surgical procedure performed to address a complication that can occur after breast implant surgery. Capsular contracture happens when the scar tissue, or capsule, that naturally forms around the implant becomes too tight or hard. This can lead to breast distortion, pain, discomfort, and aesthetic concerns.
During capsular contracture correction, the surgeon may partially or completely remove the hardened capsule (capsulectomy) and, if necessary, replace the breast implant. In some cases, a capsulotomy is performed, where the capsule is incised to release the tension without removing it. The choice of procedure depends on the severity of the contracture and the specific needs of the patient.
Capsular contracture correction is a surgical procedure performed to address a complication that can occur after breast implant surgery.
The surgery is typically done under general anesthesia, and recovery time varies depending on the complexity of the procedure. After surgery, patients may experience swelling, bruising, and discomfort, but these symptoms usually subside over time. Following the surgeon’s post-operative care instructions is crucial to ensure proper healing and reduce the risk of the contracture recurring.
Capsular contracture correction can help restore comfort and improve the appearance of the breast, but it’s important to understand that there is a possibility of recurrence. An experienced plastic surgeon can help minimize the risks and discuss the best treatment options.
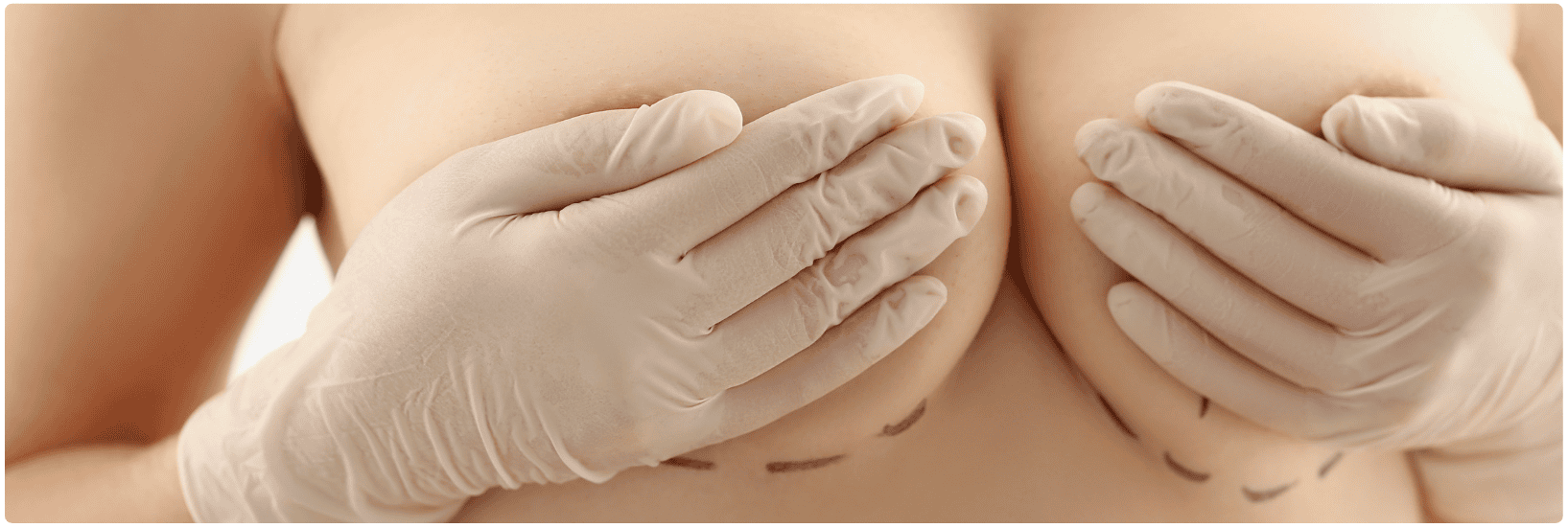
Why undergo Capsular Contracture Correction?
Capsular contracture correction is a surgical procedure designed to treat complications from breast implants, specifically when the scar tissue that forms around the implant becomes tight, hard, or painful. This condition, known as capsular contracture, can distort the shape of the breasts, causing discomfort and an unnatural appearance. People seek this corrective surgery when the contracture impacts their physical comfort or affects the aesthetic results of their breast augmentation or reconstruction.
Capsular contracture correction is a surgical procedure designed to treat complications from breast implants, specifically when the scar tissue that forms around the implant becomes tight, hard, or painful.
Capsular contracture can occur for various reasons, including infection, trauma, or the body’s natural response to a foreign object (the implant). While mild cases may cause only slight firmness, more severe cases can result in significant breast deformity, hardness, and pain. Correcting capsular contracture is important not only for cosmetic reasons but also to alleviate discomfort and restore the softness and natural feel of the breasts. For many women, undergoing this procedure helps them regain confidence and comfort after experiencing complications from their initial breast surgery.
How is Capsular Contracture Correction performed?
Capsular contracture correction surgery involves removing or modifying the tight scar tissue, also known as the capsule, that has formed around the breast implant. The procedure can be done in different ways, depending on the severity of the contracture and the patient’s goals. In some cases, the surgeon may perform a "capsulotomy," where the capsule is surgically released or cut to reduce the tightness around the implant, allowing it to sit more naturally. In more severe cases, a "capsulectomy" may be performed, which involves removing the entire capsule of scar tissue. This is typically followed by either replacing the old implant with a new one or, in some cases, removing the implant entirely if the patient no longer desires implants.
The procedure is performed under general anesthesia and usually takes one to two hours, depending on the complexity of the surgery. If the implant is being replaced, the surgeon may place the new implant in a different location, either above or below the chest muscle, to reduce the likelihood of recurrence. Additionally, surgeons may use newer implant types or specialized techniques to further minimize the risk of future capsular contracture. Post-surgery, drainage tubes may be used temporarily to help reduce fluid buildup and promote proper healing.
Recovery from capsular contracture correction usually involves some swelling, bruising, and discomfort, but these symptoms typically subside within a few weeks. Patients are advised to avoid strenuous activities for several weeks to allow the body to heal properly. Most women experience a noticeable improvement in the appearance and feel of their breasts soon after the procedure, with final results becoming more apparent as the swelling diminishes. Regular follow-up appointments with the surgeon ensure that healing progresses as expected and to monitor for any potential recurrence of the contracture.

Advanced Techniques in Capsular Contracture Correction
Modern capsular contracture correction often utilizes advanced surgical techniques to reduce recurrence. Some surgeons employ a dual-plane approach, where the implant is partially placed under the chest muscle to create more natural contours. Another innovation is the use of acellular dermal matrices (ADMs) to reinforce the breast pocket and decrease scar formation. Laser-assisted capsulotomy is also an emerging option that can minimize tissue trauma. These approaches aim to improve both aesthetic outcomes and long-term implant stability.
Risks Associated with Capsular Contracture Correction
Like any surgery, capsular contracture correction carries potential risks. Complications may include infection, bleeding, changes in nipple sensation, or asymmetry after surgery. Scar tissue may reform, especially in patients prone to fibrosis. Anesthesia-related risks should also be considered, particularly for patients with underlying health conditions. Understanding these risks helps patients make informed decisions and ensures realistic expectations for post-surgical results.
Ideal Candidates for Capsular Contracture Correction
Not every patient with capsular contracture requires surgery. Candidates who may benefit most include those experiencing:
- Severe breast hardening or pain
- Noticeable asymmetry due to the contracture
- Recurrent capsular contracture after prior surgery
- Dissatisfaction with the breast shape or contour
Patients should undergo a thorough consultation with a board-certified plastic surgeon to determine the best treatment approach and whether surgery is necessary.
Choosing the Right Implant During Correction Surgery
Selecting a suitable implant during capsular contracture correction is crucial for long-term success. Options include silicone gel implants, saline implants, or newer cohesive gel varieties. Surgeons may also consider changing the implant size, shape, or placement to prevent future complications. Choosing textured or smooth surfaces may impact recurrence rates, depending on the patient’s tissue characteristics. Proper implant selection helps enhance the overall appearance while minimizing the risk of another contracture.
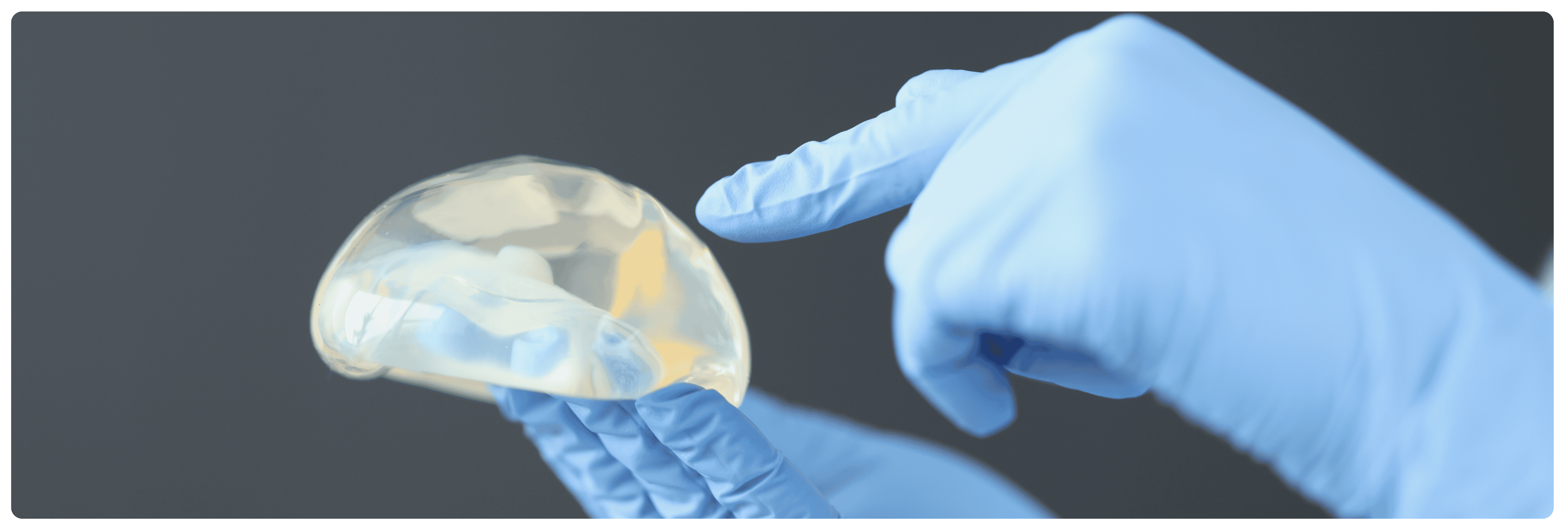
What are the benefits of Capsular Contracture Correction?
One of the main benefits of capsular contracture correction is the restoration of a natural, soft breast contour and feel. When capsular contracture occurs, the breast can become hard, misshapen, and uncomfortable, significantly affecting both appearance and physical sensation. Corrective surgery can restore the softness and symmetry of the breasts, helping women feel more confident in their appearance and more comfortable in their daily lives. Many patients find that the procedure not only improves the look of their breasts but also alleviates the pain and tightness associated with the condition.
Another important benefit is the improvement in overall comfort. Capsular contracture can cause pain or tightness, particularly in more severe cases where the implant is squeezed by the hardened capsule. This can make it difficult to wear certain clothing or bras, and it may interfere with physical activities. By removing or releasing the capsule, this surgery relieves the pressure on the implant, allowing the breasts to move more naturally and comfortably. This can significantly improve the patient’s quality of life, both physically and emotionally.
Finally, capsular contracture correction offers long-term results and can prevent further complications. Surgeons often take additional steps to minimize the risk of contracture recurrence, such as using newer implant materials or adjusting the placement of the implant. With proper post-operative care and follow-up, many patients experience a significant reduction in the likelihood of the contracture returning, allowing them to enjoy the benefits of their breast augmentation or reconstruction for many years. Overall, this procedure helps women who have experienced complications regain their desired breast appearance, comfort, and confidence.
Understanding Costs of Capsular Contracture Correction
The cost of capsular contracture correction varies based on several factors, including:
- Surgical complexity and duration
- Type of anesthesia used
- Implant replacement or additional procedures required
- Surgeon’s experience and clinic location
Understanding these factors allows patients to plan financially and select the best treatment options. While prices may vary, investing in a qualified surgeon can have a significant impact on both safety and results.

Signs and Symptoms of Capsular Contracture
Understanding the early signs of capsular contracture can help patients seek timely intervention before the condition worsens. In the initial stages, the breast may feel slightly firmer than usual, or the implant may sit higher on the chest. As the condition progresses, symptoms can include increasing tightness, a visible change in breast shape, pain or discomfort, and even asymmetry between the breasts.
Capsular contracture is often classified into four grades (Baker grades I-IV), with Grade I being a soft, natural-feeling breast and Grade IV involving significant hardness and discomfort. Recognizing these symptoms early can allow for non-surgical or minimally invasive treatments to be considered before surgical capsular contracture correction becomes necessary.
Preventing Capsular Contracture After Breast Surgery
While it’s not always possible to prevent capsular contracture, several steps can reduce the risk. Surgeons often recommend techniques such as placing the implant under the muscle (submuscular placement), using textured or more advanced implant types, and ensuring strict sterile techniques during surgery to minimize bacterial contamination.
Post-operative care is equally crucial. Massaging the breasts (if recommended by the surgeon), wearing compression garments, and avoiding strenuous activities during the initial healing period can all help lower the risk. Patients are also encouraged to attend regular follow-up appointments to monitor their healing process and detect any early signs of capsule formation.
Choosing the Right Surgeon for Capsular Contracture Correction
Selecting an experienced, board-certified plastic surgeon is essential when considering capsular contracture correction. Because this procedure can be complex—especially if scar tissue is dense or the implant has shifted—it requires advanced surgical skills and a deep understanding of breast anatomy and implant behavior.
A qualified surgeon will thoroughly assess the extent of the contracture, discuss your goals, and recommend a personalized surgical plan. Look for a specialist with a strong track record in revision breast surgeries, and don’t hesitate to ask for before-and-after photos or patient testimonials during your consultation.
What to Expect During Recovery from Correction Surgery
Recovery after capsular contracture correction varies depending on the surgical approach and the patient’s individual healing response. Most patients can return to light activities within a few days, but strenuous exercise should be avoided for several weeks. Swelling and bruising are common but usually decrease within the first few weeks.
It’s important to follow your surgeon’s post-operative instructions carefully, including taking prescribed medications, attending follow-up visits, and wearing any recommended support garments. Keeping the surgical area clean and avoiding pressure on the chest can help promote healing and reduce complications. With proper care, patients can enjoy improved comfort and breast appearance with minimal disruption to their daily lives.
Post-Surgical Care Tips for Capsular Contracture Correction
Effective post-operative care is essential for recovery and long-term results:
- Follow all instructions provided by the surgeon carefully
- Wear supportive garments as recommended
- Avoid lifting heavy objects or strenuous exercise for the prescribed period
- Attend all scheduled follow-up appointments
- Keep the incision site clean and monitor for signs of infection
Adhering to these guidelines can promote faster healing and reduce the likelihood of complications.
Non-Surgical Options to Delay Capsular Contracture
While surgery is the definitive treatment, some non-surgical approaches may help delay capsular contracture progression:
- Massage techniques, if advised by a surgeon
- Ultrasound therapy to soften the capsule
- Oral medications to reduce inflammation
- Specialized post-operative exercises to maintain breast mobility
These methods are not permanent solutions but may provide temporary relief and improve comfort before surgery becomes necessary.
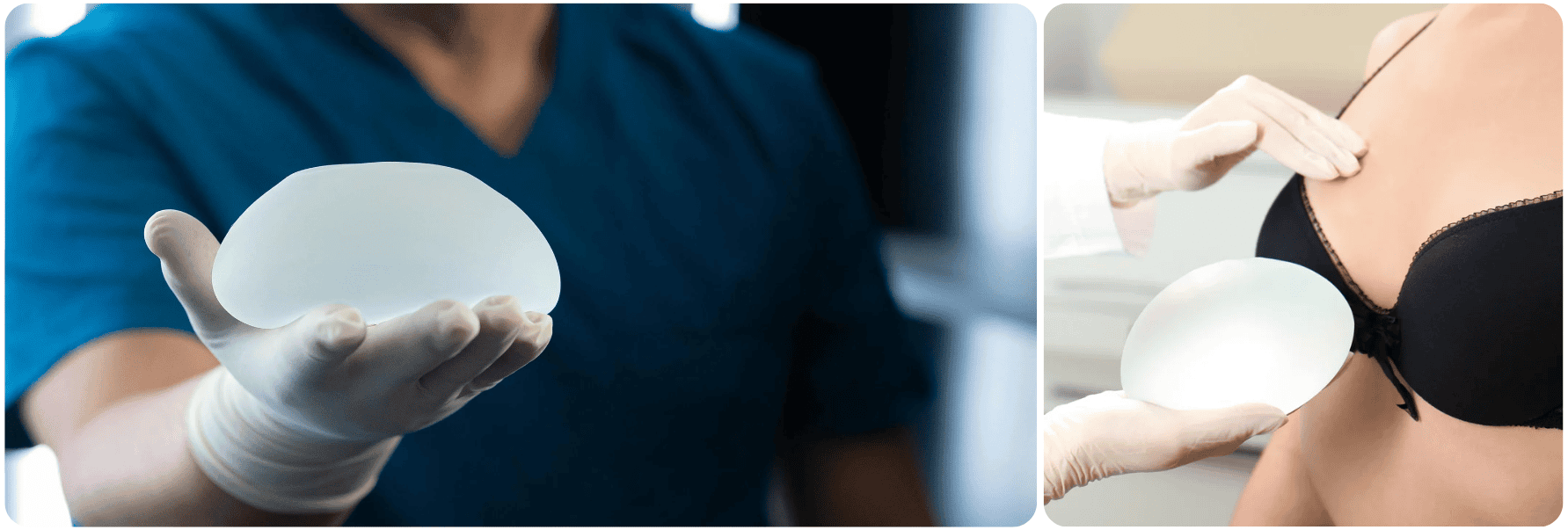
Recovery Timeline After Capsular Contracture Correction
The recovery timeline for capsular contracture correction varies depending on the complexity of the procedure. Most patients experience swelling and bruising for 2-3 weeks. Light daily activities can often be resumed after one week, while exercise or heavy lifting should be avoided for 4-6 weeks. Full results are usually visible within 3-6 months as tissues settle and scars soften. Following the recovery plan carefully ensures optimal outcomes and minimizes the risk of recurrence.
Impact of Implant Placement on Capsular Contracture
The position of the implant can influence the likelihood of capsular contracture returning. Submuscular placement, where the implant is partially under the chest muscle, often reduces recurrence compared to subglandular placement. Surgeons may also adjust the implant pocket or use specialized techniques to create a smoother environment. Choosing the optimal placement during revision surgery can improve both the aesthetic result and long-term comfort. This strategic approach is a key factor in achieving lasting correction.
Innovations in Capsular Contracture Treatment
Recent innovations in capsular contracture correction aim to reduce surgical trauma and improve results. Techniques such as endoscopic-assisted capsulotomy allow surgeons to make smaller incisions while achieving precise capsule release. Advanced imaging tools can help map the capsule accurately before surgery. Some clinics now use anti-adhesion solutions to prevent scar formation around implants. These modern methods contribute to quicker recovery, better cosmetic outcomes, and lower recurrence rates.
Capsular Contracture Correction for Reconstruction Patients
Patients who have undergone breast reconstruction may also require capsular contracture correction. Contracture can distort reconstructed breasts and affect symmetry with the natural breast. Corrective surgery can involve removing the capsule, replacing the implant, or adjusting the tissue flap used in reconstruction. Surgeons often take special care to preserve reconstructed tissues and maintain optimal aesthetics. Early intervention can prevent further complications and improve long-term results.
Preventing Recurrence of Capsular Contracture
Preventing recurrence is a critical goal of capsular contracture correction. Surgeons may use strategies such as:
- Changing implant placement from subglandular to submuscular
- Selecting newer implant types with lower contracture rates
- Using acellular dermal matrices for pocket reinforcement
- Meticulous surgical technique to minimize tissue trauma and contamination
Combining these methods can significantly lower the chances of future contracture and improve patient satisfaction.

Long-Term Considerations After Correction Surgery
After capsular contracture correction, patients should be aware of long-term considerations. Implants may still need monitoring over time for rupture, leakage, or position changes. Routine follow-up visits allow early detection of any new capsule formation. Maintaining overall breast health and reporting changes promptly ensures that corrective measures can be taken quickly. Staying informed and proactive helps maintain both aesthetic and functional outcomes.
Capsular Contracture Correction in Complex Cases
Some patients present with complex capsular contracture, such as multiple prior surgeries or severe scar tissue. In these cases, revision surgery requires advanced techniques and careful planning. Surgeons may perform a total capsulectomy combined with implant repositioning or replacement. Specialized post-operative care, including drainage management and scar therapy, is often required. Complex cases benefit most from experienced surgeons who understand the nuances of challenging breast anatomy.
Some patients present with complex capsular contracture, such as multiple prior surgeries or severe scar tissue.
Role of Antibiotics in Capsular Contracture Correction
Antibiotics play an important role in capsular contracture correction surgery. Pre-operative antibiotics reduce the risk of infection, which is a known factor in contracture development. Post-operative antibiotics may be prescribed in certain cases to prevent bacterial contamination of the implant. Following the surgeon’s instructions regarding antibiotic use can help protect against complications and support proper healing. This preventative step contributes to more predictable outcomes and fewer recurrences.


