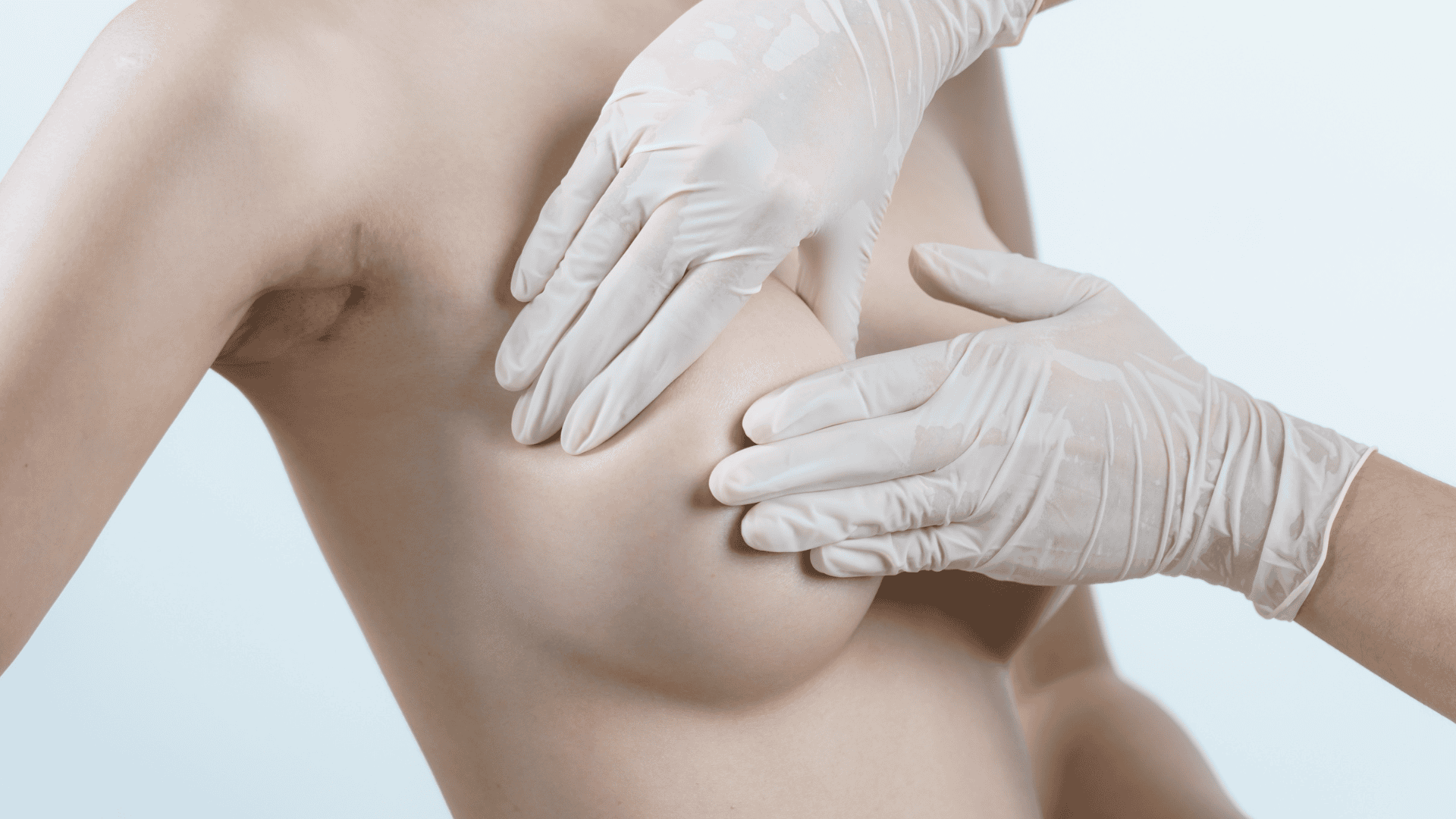
Breast-Conserving Surgery (Lumpectomy) explained in detail
- Why choose Breast-Conserving Surgery (Lumpectomy)?
- Breast-Conserving Surgery risks and considerations
- Breast-Conserving Surgery anesthesia
- How is Breast-Conserving Surgery (Lumpectomy) performed?
- Breast-Conserving Surgery surgical techniques
- Breast-Conserving Surgery cost factors
- What are the benefits of Breast-Conserving Surgery (Lumpectomy)?
- Breast-Conserving Surgery recovery process
- Breast-Conserving Surgery candidate criteria
- Breast-Conserving Surgery versus mastectomy
- Breast-Conserving Surgery preparation
- Breast-Conserving Surgery hospital stay
- Breast-Conserving Surgery follow-up care
- Breast-Conserving Surgery radiation therapy
- Breast-Conserving Surgery scar healing
- Breast-Conserving Surgery long-term monitoring
Breast-conserving surgery, also known as a lumpectomy, is a surgical procedure in which only the tumor and a small margin of surrounding healthy tissue are removed from the breast, rather than the entire breast. The primary goal of this procedure is to eliminate the cancer while preserving as much of the breast tissue as possible, maintaining the natural shape and appearance of the breast.
This surgery is often performed on women with early-stage breast cancer where the tumor is small and localized. Breast-conserving surgery is typically followed by radiation therapy to reduce the risk of the cancer returning in the remaining breast tissue. One of the key benefits of a lumpectomy is that it allows women to retain their breast, which can be important both aesthetically and emotionally.
Breast-conserving surgery, also known as a lumpectomy, is a surgical procedure in which only the tumor and a small margin of surrounding healthy tissue are removed from the breast, rather than the entire breast.
During the procedure, the surgeon carefully removes the tumor along with a rim of healthy tissue to ensure that no cancerous cells are left behind. This is known as achieving "clear margins." In some cases, the surgeon may also remove nearby lymph nodes from the underarm area to check if the cancer has spread. The size and location of the tumor, along with the overall size of the breast, can affect whether a patient is a good candidate for this type of surgery.
While breast-conserving surgery is highly effective, its suitability depends on factors such as the size and position of the tumor, the size of the breast, and whether multiple tumors are present. After surgery, radiation therapy is typically used to target any remaining cancer cells and reduce the likelihood of recurrence. The survival rates for breast-conserving surgery combined with radiation are often comparable to those of a full mastectomy, making it a widely used treatment option for women diagnosed with breast cancer.
Why choose Breast-Conserving Surgery (Lumpectomy)?
Breast-conserving surgery, also known as a lumpectomy, is a procedure in which only the tumor or abnormal tissue in the breast is removed, while preserving as much of the breast tissue as possible. This approach is often chosen by patients who are diagnosed with early-stage breast cancer or benign tumors. The key advantage of breast-conserving surgery is that it offers a solution that allows the patient to keep their breast intact, providing a less invasive option compared to a full mastectomy.
Breast-conserving surgery, also known as a lumpectomy, is a procedure in which only the tumor or abnormal tissue in the breast is removed, while preserving as much of the breast tissue as possible.
Many women prefer breast-conserving surgery because it provides a more natural appearance post-surgery, without the need for breast reconstruction. Additionally, lumpectomy patients typically experience a faster recovery and less scarring than those undergoing mastectomy. Another important factor is that for many women, breast-conserving surgery is as effective as mastectomy in treating early-stage breast cancer, as long as the tumor is adequately removed and followed by radiation therapy. This procedure allows patients to retain their body image while also successfully addressing their medical concerns, making it an appealing choice for many.
Breast-Conserving Surgery risks and considerations
Like any surgical procedure, lumpectomy comes with some risks and potential side effects. The most common include infection at the incision site, bleeding, or a temporary build-up of fluid in the breast. Radiation therapy that follows the surgery may also cause skin irritation or fatigue. Other considerations include:
👉 Changes in breast shape or size depending on the tumor location
👉 Possibility of scar tissue forming inside the breast
👉 Rare risk of the cancer not being completely removed
👉 Need for additional surgery if clear margins are not achieved
While these risks exist, most women experience smooth recoveries, especially when working closely with their healthcare team.
Breast-Conserving Surgery anesthesia
Breast-conserving surgery is almost always performed under general anesthesia to ensure comfort during the procedure. An anesthesiologist monitors vital signs throughout surgery, making adjustments as needed. Before the operation, patients discuss their medical history, allergies, and previous experiences with anesthesia to ensure a safe plan. Key points about anesthesia during lumpectomy include:
👉 General anesthesia is the standard choice for most patients
👉 Sedatives and pain medication are administered through an IV
👉 Patients remain asleep and pain-free throughout the procedure
👉 Recovery from anesthesia usually takes a few hours
👉 Nausea and grogginess are common side effects but usually short-lived
Having a clear understanding of anesthesia helps patients feel more confident and prepared before surgery.
How is Breast-Conserving Surgery (Lumpectomy) performed?
Breast-conserving surgery is typically performed under general anesthesia to ensure the patient is comfortable during the procedure. The first step in the procedure is the identification and removal of the tumor or abnormal tissue. This may be done with the assistance of imaging techniques such as mammography, ultrasound, or MRI, which guide the surgeon in accurately locating the tumor. The surgeon makes a small incision in the breast and carefully excises the tumor, along with a small margin of healthy tissue around it to ensure that all cancerous cells have been removed. The amount of tissue removed depends on the size and location of the tumor, but the goal is always to preserve as much healthy tissue as possible.
Breast-conserving surgery is typically performed under general anesthesia to ensure the patient is comfortable during the procedure.
In some cases, the surgeon may remove nearby lymph nodes to check if the cancer has spread. After the tumor is removed, the incision is closed, and the breast is reconstructed to maintain its shape. Most women are able to go home the same day or after a short stay in the hospital. While the procedure is less invasive than a mastectomy, some form of radiation therapy is often recommended afterward to ensure that any remaining cancer cells are destroyed and to reduce the risk of recurrence.
Breast-Conserving Surgery surgical techniques
Modern advances have led to different techniques in breast-conserving surgery, making it more precise and effective than ever. Surgeons may use advanced imaging during the procedure to guide them and ensure complete removal of the tumor. In some cases, oncoplastic surgery techniques are combined with lumpectomy to improve cosmetic results.
These techniques allow surgeons to reshape the breast while removing cancerous tissue, offering both medical and aesthetic benefits. Such innovations have expanded the number of women who can be considered good candidates for lumpectomy. By blending cancer treatment with reconstructive methods, modern surgical techniques help women achieve the best of both health and appearance.
Breast-Conserving Surgery cost factors
The cost of breast-conserving surgery varies depending on several factors, including the location of the clinic, the surgeon’s experience, and whether additional procedures such as lymph node removal are required. Radiation therapy and follow-up care are usually additional expenses that need to be considered. Factors that can influence the cost include:
👉 Type of healthcare system or insurance coverage
👉 Whether advanced imaging or oncoplastic techniques are used
👉 Hospital stay duration, if required
👉 Medications and anesthesia fees
👉 Post-surgery follow-up and radiation sessions
Understanding these cost factors helps patients prepare financially and explore treatment options that best suit their needs.
What are the benefits of Breast-Conserving Surgery (Lumpectomy)?
The primary benefit of breast-conserving surgery is the ability to remove the tumor while preserving the majority of the breast tissue, allowing patients to maintain a more natural appearance post-surgery. This can be especially important for women concerned about body image and self-esteem following a breast cancer diagnosis. Unlike a mastectomy, which involves removing the entire breast, lumpectomy offers a less invasive approach with a shorter recovery time, fewer complications, and a smaller incision.
Many women also find that they experience less pain and swelling after breast-conserving surgery compared to a full mastectomy. Additionally, for women with early-stage breast cancer, lumpectomy can be just as effective as mastectomy in treating the cancer, as long as it is followed by radiation therapy, which helps reduce the risk of the cancer returning. Another advantage is that the procedure often allows for a quicker return to daily activities and work, as recovery times are generally shorter.
Finally, breast-conserving surgery helps women preserve their overall quality of life while effectively addressing their medical needs, offering both emotional and physical benefits in the fight against breast cancer.
Breast-Conserving Surgery recovery process
The recovery process after breast-conserving surgery (lumpectomy) is usually shorter than after a full mastectomy, but it still requires care and patience. Most women are able to return home the same day, though some may need a brief hospital stay depending on the complexity of the procedure. The incision site may feel tender and swollen for a few weeks, and patients are advised to follow their surgeon’s post-operative instructions carefully.
It is important to avoid heavy lifting and intense physical activity for a certain period to allow proper healing. Many patients also find that wearing a supportive bra during recovery helps minimize discomfort and maintain breast shape. Over time, the majority of women notice that their breast looks and feels relatively natural, which is one of the reasons lumpectomy is often a preferred choice.
Breast-Conserving Surgery candidate criteria
Not every patient with breast cancer is an ideal candidate for lumpectomy. Surgeons usually recommend this procedure for women with early-stage breast cancer where the tumor is relatively small compared to the breast size. A single tumor, rather than multiple tumors in different areas of the breast, is generally a key requirement. Patients must also be willing to undergo radiation therapy after surgery, as this is a crucial part of the treatment plan. Candidates are often evaluated based on:
👉 Tumor size and location
👉 Overall breast size and shape
👉 Presence of additional tumors
👉 General health and ability to tolerate anesthesia
👉 Willingness to commit to follow-up treatments
By carefully assessing these factors, surgeons can ensure the best possible outcome for each patient.
Breast-Conserving Surgery versus mastectomy
One of the most common questions women ask when diagnosed with breast cancer is whether they should choose breast-conserving surgery or a mastectomy. Both procedures are effective in treating cancer, but the decision depends on medical, cosmetic, and personal factors. Lumpectomy allows women to keep most of their breast tissue intact, but it requires radiation afterward.
A mastectomy, on the other hand, removes the entire breast and may eliminate the need for radiation in some cases. While survival rates between the two approaches are often comparable, lumpectomy typically results in shorter recovery time and less invasive surgery. Understanding these differences helps patients make an informed decision that best suits their lifestyle and health needs.
Breast-Conserving Surgery preparation
Preparing for breast-conserving surgery involves both medical and personal steps to ensure a smooth experience. Surgeons usually request pre-operative imaging, such as MRI or ultrasound, to precisely locate the tumor. Patients may also need routine blood tests and a general health assessment. Common preparation steps include:
👉 Avoiding certain medications like blood thinners before surgery
👉 Stopping smoking to improve healing
👉 Arranging for someone to drive you home after the procedure
👉 Wearing loose, comfortable clothing on the surgery day
👉 Discussing any allergies or medical conditions with your surgeon
By following these steps, patients can help minimize risks and ensure the surgery proceeds safely.
Breast-Conserving Surgery hospital stay
The majority of women undergoing lumpectomy do not need a long hospital stay. In fact, many patients are discharged the same day, especially if the surgery is straightforward and there are no complications. However, in some cases where lymph nodes are removed or additional procedures are needed, an overnight stay may be recommended. The decision depends on the patient’s health, the complexity of the surgery, and the surgeon’s assessment. Most women appreciate the fact that lumpectomy often requires minimal time in the hospital, allowing them to continue recovery in the comfort of their own home. This shorter hospital stay is another advantage of breast-conserving surgery compared to more invasive options.
Breast-Conserving Surgery follow-up care
After breast-conserving surgery, follow-up care is a critical part of treatment. Regular check-ups ensure that healing is progressing well and that there are no complications. Surgeons typically monitor the incision site and may order imaging tests to confirm that all cancerous tissue was successfully removed. Follow-up care often includes:
👉 Post-surgery wound care instructions
👉 Scheduled visits with the surgeon and oncologist
👉 Radiation therapy sessions
👉 Medication or hormone therapy, if required
👉 Long-term monitoring with mammograms or MRIs
By following the recommended care plan, patients significantly reduce the chances of recurrence and maintain long-term breast health.
Breast-Conserving Surgery radiation therapy
Radiation therapy is almost always part of the treatment plan after lumpectomy. This therapy uses high-energy beams to destroy any remaining cancer cells in the breast, lowering the risk of recurrence. Radiation is typically delivered daily over several weeks, depending on the treatment plan. Key facts about radiation after lumpectomy include:
👉 It is highly effective in preventing cancer return
👉 Treatment is usually painless but may cause skin redness or fatigue
👉 Sessions are short, often lasting less than 30 minutes
👉 Technology allows precise targeting to protect surrounding tissues
👉 Long-term side effects are rare but may include slight breast firmness
Radiation therapy is an essential partner to breast-conserving surgery, ensuring the best long-term outcomes.

Breast-Conserving Surgery scar healing
The appearance of scars after breast-conserving surgery is often minimal compared to larger operations. Surgeons usually make careful incisions in less visible areas, such as along the natural curves of the breast. Over time, scars typically fade and become less noticeable, especially when patients follow proper wound care instructions. Moisturizing creams, silicone sheets, or gentle massages can sometimes help improve scar healing.
Some women may experience firmness or slight changes in skin texture, but these usually soften with time. The majority of patients are pleased with the aesthetic results, as the breast maintains its natural shape despite the removal of cancerous tissue.
Breast-Conserving Surgery long-term monitoring
Even after successful lumpectomy and radiation therapy, long-term monitoring is necessary to ensure continued breast health. Patients are usually advised to have regular mammograms and physical examinations. Early detection of any new changes is crucial for ongoing prevention. Long-term monitoring typically involves:
👉 Routine imaging tests such as mammograms or MRIs
👉 Regular consultations with the oncologist
👉 Self-examinations at home to detect changes
👉 Lifestyle recommendations to support overall health
👉 Keeping records of treatments and test results for future reference
This structured monitoring plan provides reassurance and allows healthcare providers to act quickly if new concerns arise.


